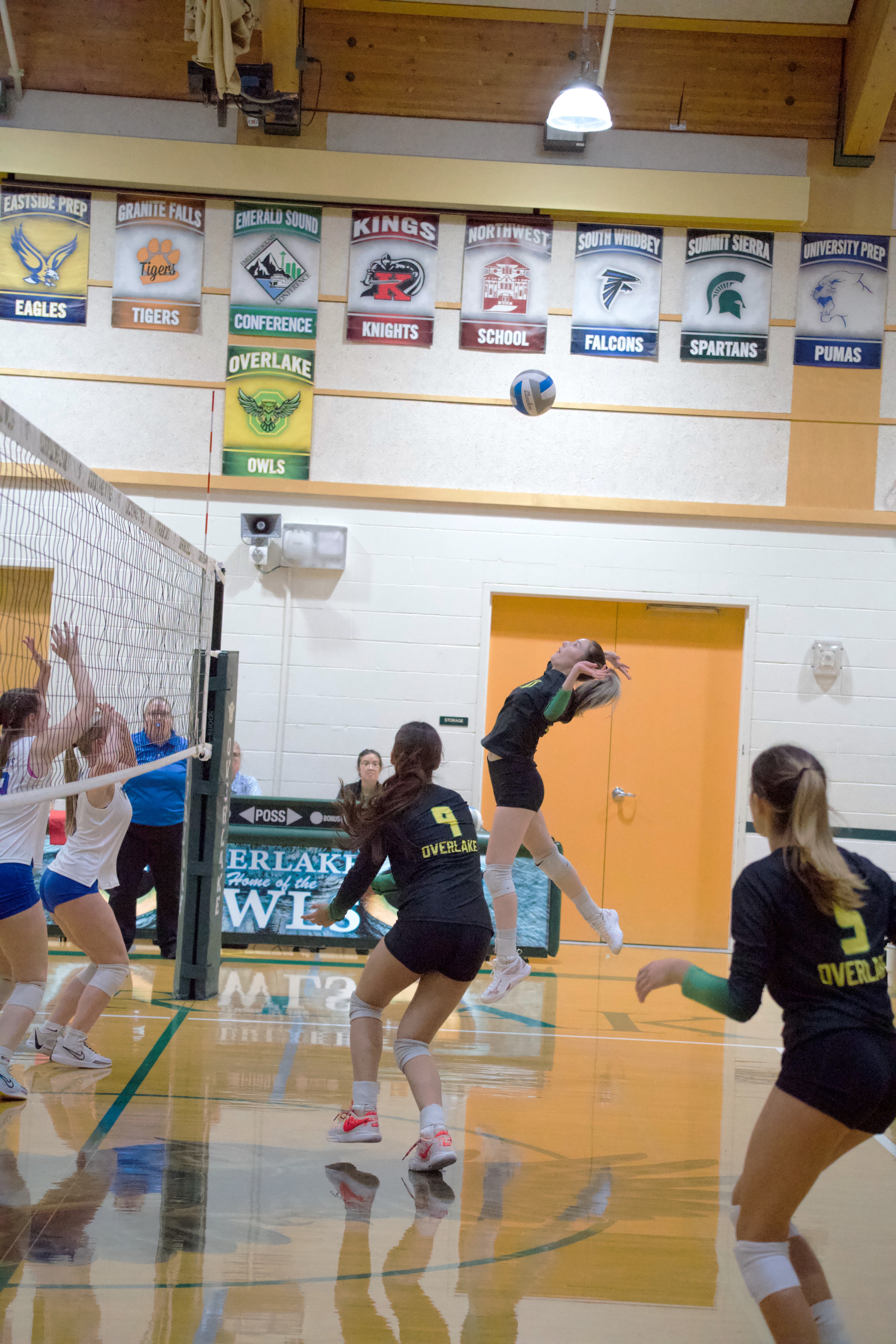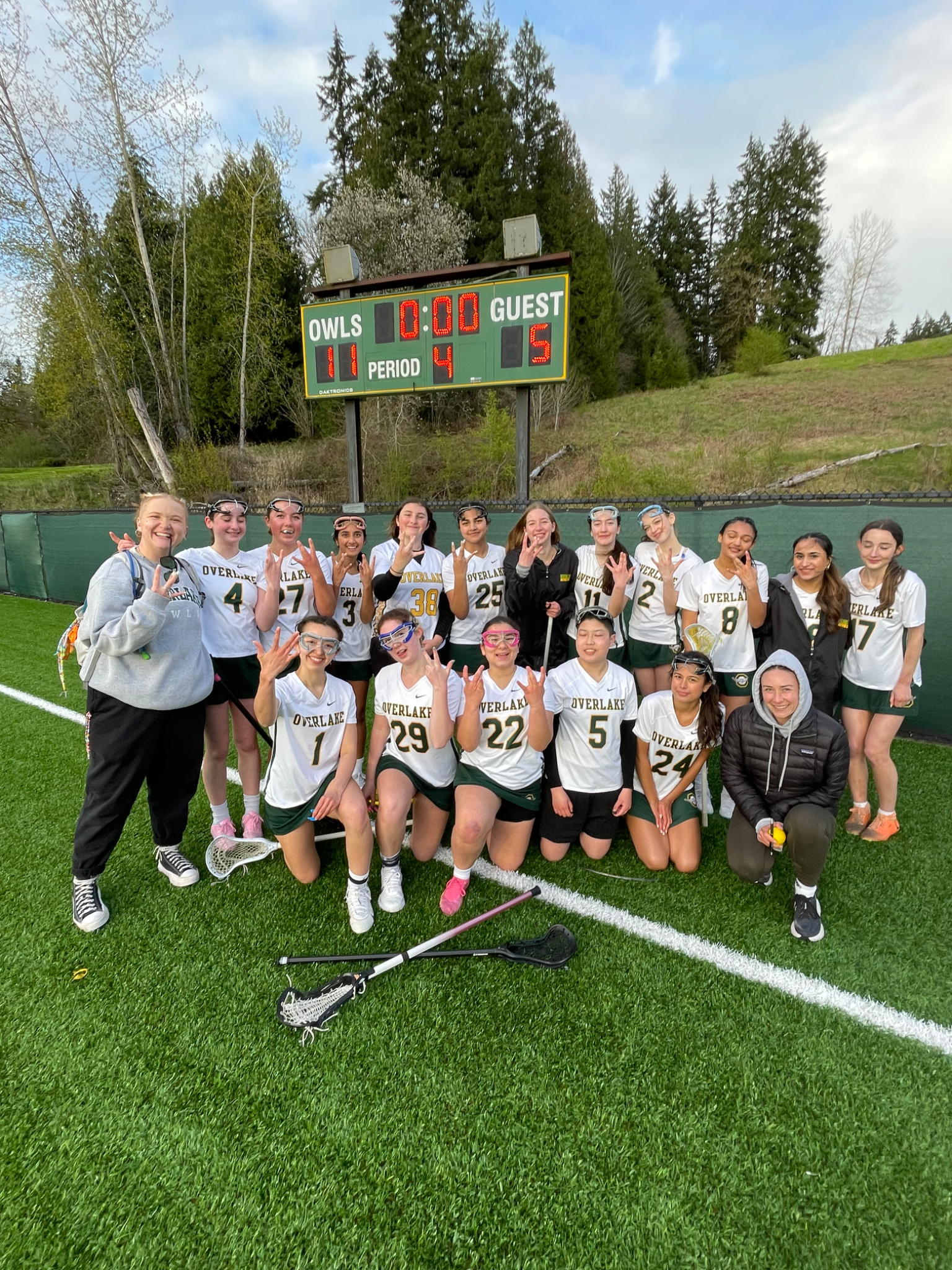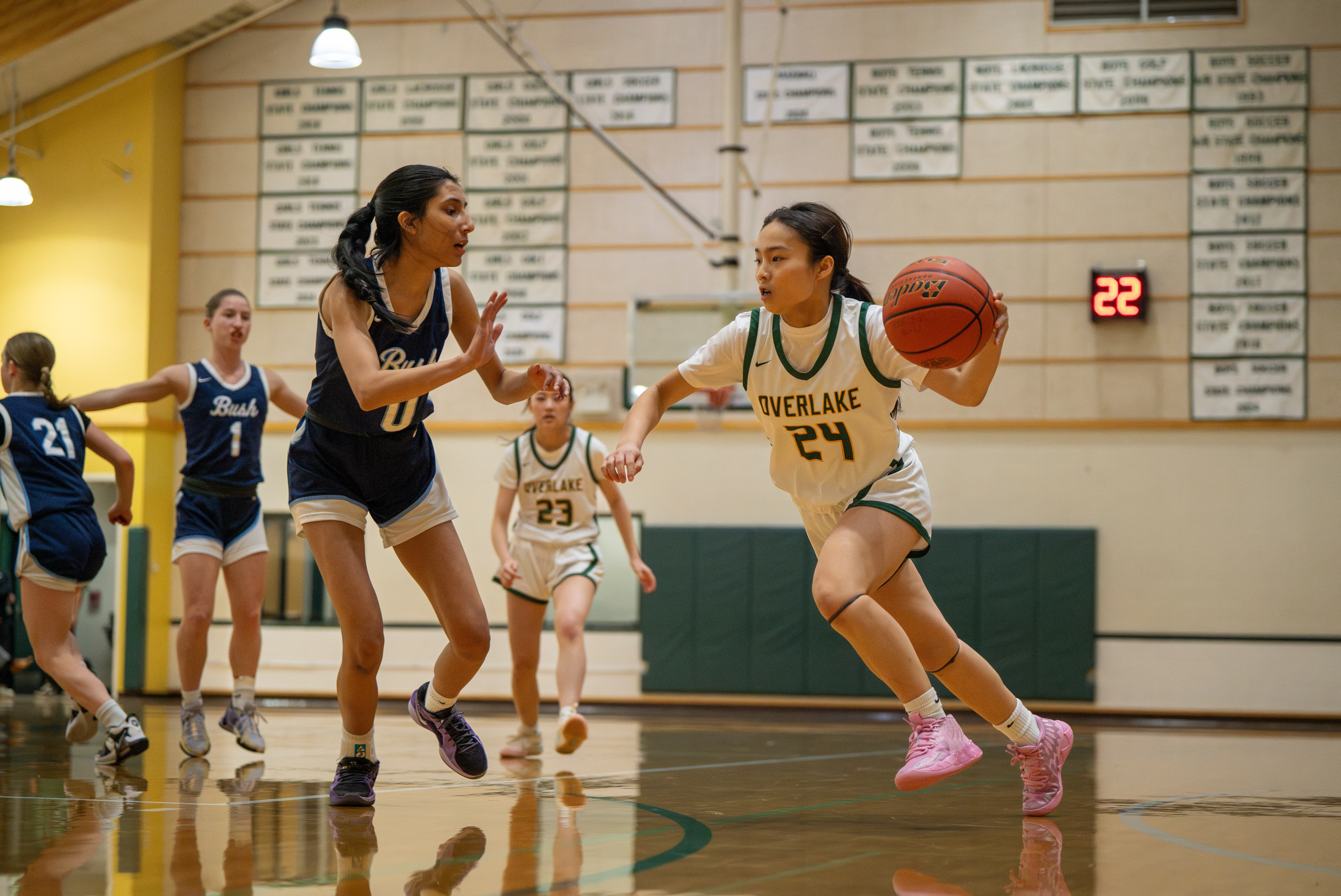Forging character through competition.
At Overlake, athletics is about more than winning games; it's about growing as people and forging bonds between teammates as they develop hard-earned life skills. Students who participate in sports not only yield friendships and leadership abilities, they also maintain strong academic performance and fortify healthy habits that serve them well into adulthood. For many learners, the experience of being on a team becomes a treasured opportunity and a memorable time in their lives.
Teaching character in a fun, competitive environment.
Character is who you are when no one's watching. It's built through challenges, especially when the outcome isn't certain. This is what Overlake Athletics is all about. In the classroom, you can study for a test and feel prepared; sports are different. You face actual opponents, compete in tough situations, and perform in front of your teammates and community. It's challenging, but it's how we grow. Whether you win or learn from a loss, you're moving forward. We're here to support students through it all, celebrating victories and learning from setbacks—together.
Playing more than one sport has huge benefits.
Studies show that students who play multiple sports perform better athletically, experience fewer injuries, and continue competing longer. At Overlake, we encourage students to try different sports throughout the year. These athletes build new skills, form friendships across teams, and recognize what they love. More than 80% of our students participate in athletics, and most play more than one sport each year.

Sports are more than just games to us.
We're proud to be competitive. In 2024, Overlake was named the #1 athletic department in the state for our size. Year after year, our boys and girls teams rank among the top in Washington. We foster character, which evolves into building champions. In the past decade alone, we've earned state titles in Soccer (4), Tennis (6), Golf (2), and Baseball (1). Our teams have made deep runs at state in Basketball, Volleyball, Lacrosse, Ultimate, and Cross Country. Every program sets high goals, and we work diligently every day to achieve them.
Student-athletes find their edge at Overlake.
With 75 acres of campus, our facilities elevate the athletic experience and feature:
- Four (4) fields for Soccer, Lacrosse, and Ultimate
- Two (2) full-size gymnasiums for Basketball and Volleyball
- Six (6) Tennis courts (including two indoor)
- Miles of trails for Cross Country
- A state-of-the-art fitness center
- Access to nearby Baseball fields and Golf courses
Overlake athletes go on to compete at the next level more often than the national average, joining NCAA Division I, II, and III programs across top conferences. Our student-athletes consistently earn higher GPAs than their peers, thanks to learning early how to balance academics and athletics with the support of coaches and teachers. Behind it all is our coaching staff: experienced mentors who've often played at the college level themselves, and many of whom have been building their programs here for over a decade.